Michael Liddle , General Manager – Namoli Healthcare
Michael has been in the commercial cleaning and facilities management industry since 1991, bringing 34 years of hands-on and leadership experience. He has specialised in healthcare cleaning since…
View Full ProfileUnder the strengthened Aged Care Quality Standards, which replaced the previous standards in November 2025, aged care standard 4 now covers the environment. In practical terms, providers need to keep facilities clean, safe, comfortable, easy to move through, supported by safe equipment, and backed by an effective infection prevention and control system. If your team still uses the old wording, the key change is simple: what sat under Standard 5 in the previous framework now sits under Standard 4, with infection prevention made much more explicit.
What This Means Inside an Aged Care Facility
For facility managers and operational leaders, the standard is not really about presentation. It is about whether the site is being actively controlled. That includes clear corridors, safe bathrooms, functioning handrails, serviced hoists, clean and dirty utility separation, stocked PPE points and equipment that is safe to use when staff need it.
The strongest providers do not treat this as a cleaning issue alone. They treat it as a joint responsibility across facilities, care, maintenance, infection control and governance.
Step 1: Start With Risk Mapping, Not Just a Cleaning Roster
One of the most practical ways to improve a facility quickly is to walk the environment as if you were tracing risk, not appearance. A spotless foyer means very little if bathroom floors become slippery after peak use, if storage rooms are overcrowded, or if mobility equipment is left in a corridor that should remain clear for residents and emergency access.
As a general guide, facility managers should review all areas, like resident rooms, nurse stations, and storage areas, as separate risk zones. Each space has its own hazards, traffic patterns and cleaning frequency requirements. When facilities map the building this way, they are far more likely to catch issues such as blocked exits, broken dispensers, damaged seating, poor ventilation, inconsistent signage or missing hand hygiene points before they become incidents.
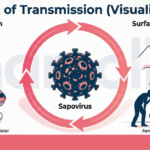
Below is a visual risk map that can be used during walk-throughs:

The infographic above turns the section into a practical scan of movement patterns, touchpoints, wet areas, utility separation, waste controls and access routes so teams can spot risks quickly and escalate faults before they affect residents or staff.
Risk mapping reinforces an important point: workplace safety is inseparable from resident safety. If workers have to manoeuvre heavy carts through cluttered hallways, if chemicals are stored poorly, or if equipment is unreliable, the risk flows directly to residents, visitors and the continuity of care.
Step 2: Turn the Risk Map Into Daily Infection Control Routines
Once a provider has mapped where risks sit, the next step is to decide what safe practice looks like in each zone and make that routine for every shift. The strengthened guidance for Outcome 4.2 on infection prevention and control requires more than having policies on file. Providers need an infection prevention and control system that workers can follow consistently in the real environment.
In practical terms, that means linking each risk area to a clear control. Wet bathrooms may need more frequent cleaning and slip-response checks. Dining rooms and communal lounges may need stricter touchpoint disinfection and better hand hygiene access. Clean and dirty utility areas need firm workflow separation so tools, linen and waste do not cross paths. PPE stations, escalation triggers, outbreak procedures and supervision should all sit where the mapped risk actually occurs, not only in training documents.
This is where many providers either strengthen the environment or lose control of it. A room can look clean and still be unsafe if the workflow is wrong. For example, a dining room floor may shine, but if the same cloths or mop heads were already used in en-suites or sluice-adjacent spaces, the process has created cross-contamination risk. By contrast, a colour-coded system backed by staff training and spot checks turns risk mapping into safer daily behaviour, not just better presentation.
Step 3: Maintain Equipment and the Physical Environment Before Faults Become Incidents
After daily workflows are defined, the third step is to make sure the environment and equipment can reliably support them. Providers sometimes treat maintenance as a separate operational issue, but under the aged care standard 4, it is part of maintaining a safe and healthy environment. Beds, pressure care equipment, mobility aids, shower chairs, handrails, nurse call buttons, medication trolleys and cleaning tools all affect whether residents and staff can move safely through the day.
This is also the point where prevention matters more than reaction. A loose toilet rail is not only a maintenance job, it is also a fall risk. A damaged wheelchair cushion affects comfort, skin integrity and dignity. An unclean or poorly maintained hoist is both an infection risk and a manual handling hazard. Once risk mapping has shown where the pressure points are, providers should translate that into routine servicing, faster defect reporting, clear accountability and repair timeframes that match the seriousness of the risk.
In other words, step 3 is about closing the loop. If step 1 identifies hazards and step 2 sets the right controls, step 3 keeps the building, fixtures and equipment in a condition that allows those controls to keep working every day.
The Best Systems Make Compliance Easy to Prove
Auditors and managers alike need to see more than intent. They need evidence that the system is functioning in the real world. The table below shows the kind of operational proof that supports a safe and healthy environment in aged care.
| Operational area | What good practice looks like | Evidence a provider should be able to show |
| Environmental cleaning | Cleaning frequencies match the risk level of each area, with clean-to-dirty workflows and clear zoning. | Cleaning schedules, completed checklists, spot-audit records, and corrective actions. |
| Infection prevention and control | Hand hygiene, PPE use, waste handling and outbreak actions are followed consistently. | IPC policies, staff training records, PPE stock checks, outbreak plans, and review notes. |
| Equipment management | Resident and staff equipment is safe, appropriate, cleaned correctly and serviced on time. | Maintenance logs, service reports, fault reports, and replacement records. |
| Environmental risk management | Hazards are identified early and acted on before they harm residents or staff. | Risk assessments, incident reports, near-miss reporting, and follow-up actions. |
| Workforce practice | Staff know which standards apply in their work area and can escalate concerns quickly. | Induction records, competency checks, toolbox talks, and supervision notes. |
When these records are up to date, compliance conversations become far easier. More importantly, the facility is less dependent on memory, individual heroics or last-minute preparation before a review.
Outbreak Response Shows Whether the System Works
A practical real-world example comes from the Australian Government’s guidance on managing infectious diseases in aged care and managing infectious respiratory diseases in aged care. When providers face flu, RSV, COVID-19 or gastro outbreaks, they are expected to move beyond routine cleaning and activate a broader response. That typically includes stricter hand hygiene, more frequent cleaning of bedrooms, communal areas and high-touch surfaces, appropriate use of masks, gloves and gowns, isolation of affected residents where needed, and clear communication with families and visitors.
This matters because it shows what a safe environment really is. It is not a static condition. It is the provider’s ability to recognise risk quickly, change cleaning intensity, support workers properly and communicate clearly without losing sight of residents’ dignity and daily needs.
The same principle applies outside outbreak periods. If a provider cannot scale up safely during higher-risk periods, the underlying system is usually too fragile even in normal operations.

Train, Check and Improve your facility
At Namoli Healthcare, our teams are trained in the real environments they work in, with strict attention to clean-to-dirty workflows, PPE use, touchpoint hygiene, zoning discipline and resident-facing risks. That training is backed by regular inspections, environmental audits and hygiene verification, so performance is checked, not assumed.
If you want to strengthen your approach to aged care standard 4, Namoli Healthcare can help you review your workflows, infection control routines and auditing processes, including ATP-based hygiene verification, so your facility is not only visibly clean but operationally defensible.

Michael Liddle , General Manager – Namoli Healthcare
Michael has been in the commercial cleaning and facilities management industry since 1991, bringing 34 years of hands-on and leadership experience. He has specialised in healthcare cleaning since…
View Full ProfileRelated Posts

Michael Liddle , General Manager – Namoli Healthcare
Michael has been in the commercial cleaning and facilities management industry since 1991, bringing 34 years of hands-on and leadership experience. He has specialised in healthcare cleaning since…
View Full Profile

Michael Liddle , General Manager – Namoli Healthcare
Michael has been in the commercial cleaning and facilities management industry since 1991, bringing 34 years of hands-on and leadership experience. He has specialised in healthcare cleaning since…
View Full Profile

Michael Liddle , General Manager – Namoli Healthcare
Michael has been in the commercial cleaning and facilities management industry since 1991, bringing 34 years of hands-on and leadership experience. He has specialised in healthcare cleaning since…
View Full Profile